Impact Factor ISSN: 1449-2288
Int J Biol Sci 2020; 16(9):1658-1675. doi:10.7150/ijbs.43447 This issue Cite
Research Paper
Is intensive glucose control bad for critically ill patients? A systematic review and meta-analysis
1. Trauma Research Center, Fourth Medical Center of the Chinese PLA General Hospital, Beijing 100048, People's Republic of China.
2. Department of Burn Surgery, Changhai Hospital, the Second Military Medical University, Shanghai 200433, People's Republic of China.
3. Department of Critical Care Medicine, Fuxing Hospital, Capital Medical University, Beijing 100038, People's Republic of China.
*Ren-qi Yao, Chao Ren and Guo-sheng Wu have contributed equally to this manuscript.
Abstract
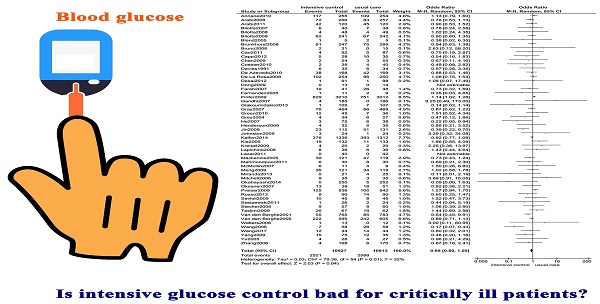
Background: The monitoring and management of blood glucose concentration are standard practices in critical settings as hyperglycaemia has been shown close association with poorer outcomes. Several meta-analyses have revealed that intensive glucose control has no benefit in decreasing short-term mortality among critically ill patients, while the studies these meta-analyses have incorporated have been largely divergent. We aim to perform a more comprehensive meta-analysis addressing this problem to provide stronger evidence.
Methods: We conducted comprehensive searches for relevant randomized controlled studies in online databases, including the Cochrane Library, EMBASE, and PubMed databases, up to September 1, 2018. The clinical data, which included all-cause mortality, severe hypoglycemia, need for RRT, infection resulting in sepsis, ICU mortality, 90-day mortality, 180-day mortality, and hospital and ICU lengths of stay, were screened and analyzed after data extraction. We applied odds ratios (ORs) to analyze dichotomous outcomes and mean differences for continuous outcomes with a random effects model.
Results: A total of 57 RCTs involving a total of 21840 patients were finally included. Patients admitted to the ICU who underwent intensive glucose control showed significantly reduced all-cause mortality (OR: 0.89; 95% CI: 0.80-1.00; P=0.04; I2=32%), reduced infection rate (OR: 0.65, 95% CI: 0.51-0.82, P=0.0002; I2=47%), a lower occurrence of acquired sepsis (OR: 0.80, 95% CI: 0.65-0.99, P=0.04; I2=0%) and shortened length of ICU stay (MD: -0.70, 95% CI: -1.21--0.19, P=0.007, I2=70%) when compared to the same parameters as those treated with the usual care strategy. However, patients in the intensive glucose control group presented with a significantly higher risk of severe hypoglycemia (OR: 5.63, 95% CI: 4.02-7.87, P<0.00001; I2=67%).
Conclusions: Critically ill patients undergoing intensive glucose control showed significantly reduced all-cause mortality, length of ICU stay and incidence of acquired infection and sepsis compared to the same parameters in patients treated with the usual care strategy, while the intensive glucose control strategy was associated with higher occurrence of severe hypoglycemic events.
Keywords: intensive glucose control, critical illness, sepsis, meta-analysis

 Global reach, higher impact
Global reach, higher impact